|
What is the differential diagnosis?
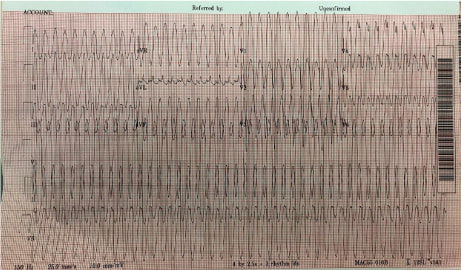
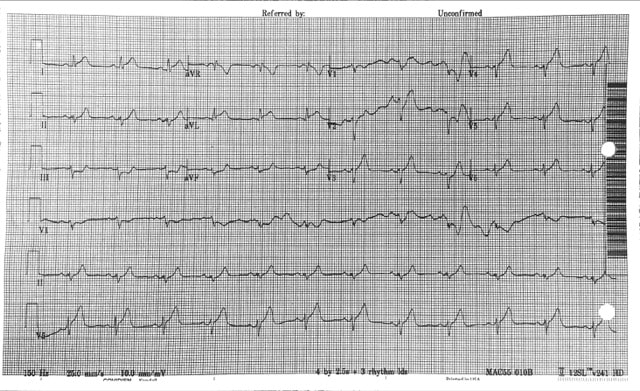
When approaching an EKG with tachycardia, one should first determine: is the QRS complex wide or narrow? And is the rhythm is regular or irregular? This patient’s EKG is regular with a wide QRS complex. Differential Diagnosis - Ventricular Tachycardia, SVT with Aberrancy (Bundle Branch Block or accessory pathway) or paced rhythm. No pacer spikes are seen which leaves VT and SVT with Aberrancy. A number of decision aid tools exist to assist in distinguishing (Brugada is most common) but are cumbersome. What's the final diagnosis?
Wide complex tachycardia likely Idiopathic Monomorphic VT originating from the RVOT. VT = QRS complexes originating in ventricle and > 30 second duration. < 30 second = NSVT. VT is classified as monomorphic (no beat to beat variation in QRS complex morphology) and polymorphic. VT can have ischemic or idiopathic etiologies. This 19 yo was unlikely to have ischemic heart disease. Management?
General Rule - Treat wide complex tachycardias as VT and cardioversion is always the safest option. Per ACLS STABLE patient with wide complex tachycardia that is REGULAR → an adenosine challenge can be attempted. This will terminate SVT and some Idiopathic VTs (eg RVOT). If unsuccessful ⇒ Procainamide Take home points:
1. Differing VT from SVT with aberrancy is not essential. It is always safest to treat as VT.
2. An adenosine challenge may be attempted for WCT only if the following two conditions are met: The patient is STABLE & The rhythm is REGULAR Sources: Link MS, Berkow LC, Kudenchuk PJ et al. Part 7: Adult Advanced Cardiovascular Life Support: 2015 American Heart Association Guidelines Update for Cardiopulmonary Resuscitation and Emergency Cardiovascular Care. Circulation 2015; 132:S444
0 Comments
What is the diagnosis?
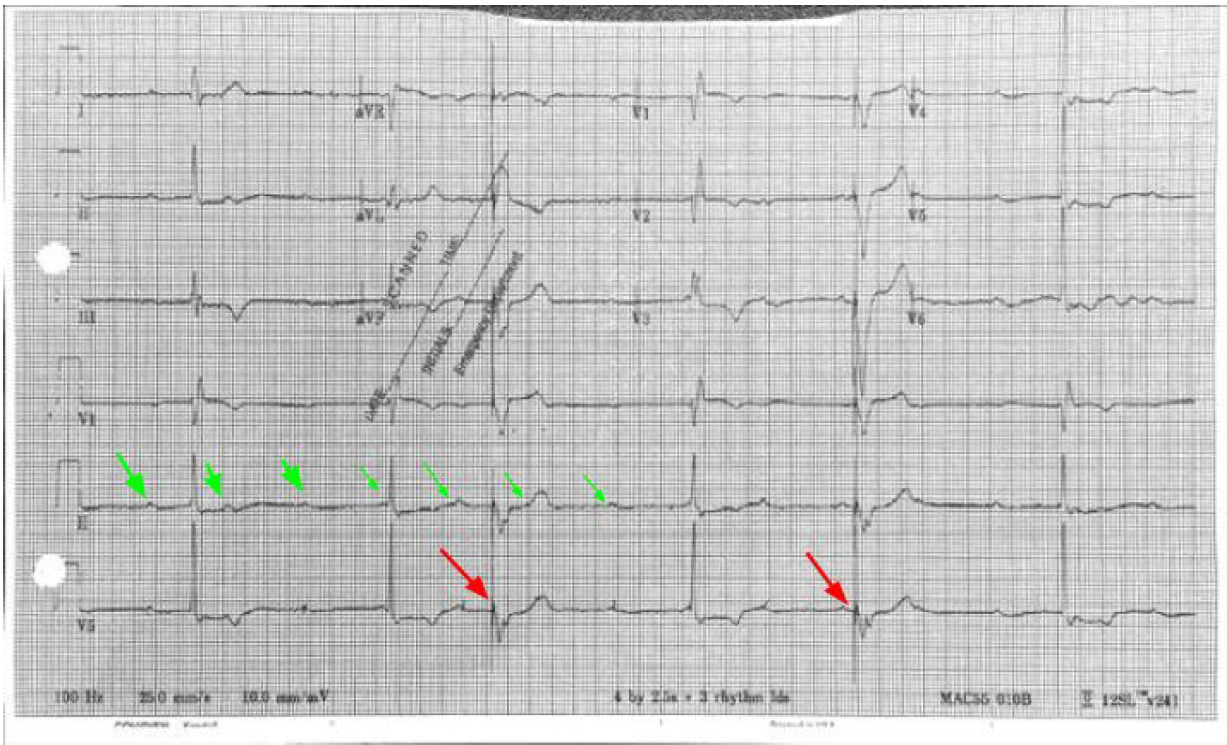
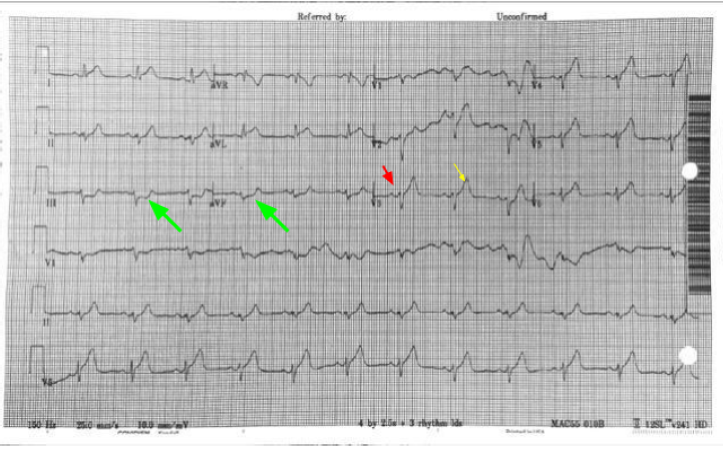
3rd Degree AV Block (Complete Heart Block) - Look at the rhythm strip and notice there is no relation between the P waves (Green Arrows) and QRS complexes which diagnoses 3rd Degree. It helps to get a piece of paper (calipers if you have) and measure the P waves. They can often be buried in the T wave or QRS complex. It is not 2nd Degree AV Block because both Mobitz I (progressively prolonged PR interval before dropped QRS) and Mobitz II (intermittent AV Block) will show some pattern of relation between the P wave and QRS complex. The escape rhythm is narrow and thus a junctional escape rhythm indicating the block is above the bundle of his. A wide complex would indicate a block at or below the bundle of His and ventricular escape rhythm. Name some possible etiologies
Etiologies: Ischemia (especially inferior MI), Medications (CCB, Beta blockers etc.) Hyperkalemia, and ask about travel and send a Lyme titer if pertinent or you’re feeling fancy **Look closely at the EKG you’ll see pacemaker spikes (Red Arrows) which are followed by ventricular capture. The patient had a PPM which had not been check in > 10 years and battery failure. Thus the pacemaker was not firing** What is the diagnosis?
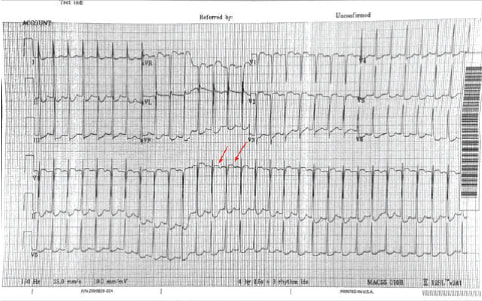
This is a narrow complex regular tachycardia. The differential diagnosis includes - sinus tachycardia, atrial flutter, paroxysmal supraventricular tachycardia PSVT which includes AVNRT - AV nodal reentrant tachycardia and AVRT (Atrioventricular Reciprocating Tachycardia), atrial tachycardia, irregular narrow complex tachycardias would include MAT (Multifocal Atrial Tachycardia) and Atrial Fibrillation. The most commonly seen etiology is PSVT. There do not appear to be P waves. However it is difficult to definitively rule out the other etiologies. One must always consider Atrial Flutter with 2:1 block when the HR is around 150. Best lead to see P wave activity is V1 (here red arrows show some blips which may be buried Ps) Is there a role for adenosine?
Adenosine will frequently terminate a PSVT and unmask underlying atrial flutter so can often be diagnostic Name an initial non-pharmacologic intervention
Vagal maneuvers. Consider using a 10 cc syringe and asking the patient to blow the plunger out ( Lin ALiEM 2012 ). Additionally there may be improved success with vagal maneuvers using postural modification as described in the REVERT Trial ( Wiki EM Summary ) Take Home Points
1. Always consider Atrial Flutter with 2:1 conduction if the HR is around 150s
2. Adenosine can be therapeutic (terminating PSVT) and and diagnostic (unmasking P waves) 3. Consider postural modification to vagal maneuvers Resources: Lin,Michelle (2012,June26) https://www.aliem.com/2012/06/tricks-of-trade-valsalva-maneuver-by/ Brady WJ, Laughrey TS, Ghaemmaghami CA. Cardiac Rhythm Disturbances. In: Tintinalli JE, Stapcyznski JS, Ma OJ, Yealy DM, Meckler CD, Cline DM, editors. Tintinalli’s Emergency Medicine: A Comprehensive Study Guide. 8th ed. McGraw-Hill; 2011. Appelboam A. et al. Postural modification to the standard Valsalva manoeuvre for emergency treatment of supraventricular tachycardias (REVERT): a randomised controlled trial. Lancet 2015 Oct 31;386(10005):1747-53 45 M presents to the ED with lightheadedness after his LVAD “Low Flow” alarm sounded. He has a normal mental status, and MAP ~ 65 mmhg What is the rhythm?
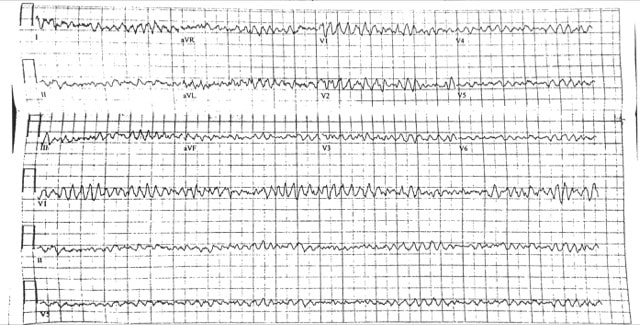
Ventricular Fibrillation. There are no P waves nor organized QRS complexes. This distinction between coarse and fine V Fib is irrelevant. In theory fine V Fib indicates it has been a longer duration but management is not different. You may look at the EKG and question whether the patient has Torsades. The initial distinction is irrelevant as the patient is likely unstable / pulseless and needs electricity. Torsades can only be diagnosed with prolonged QT on the patient’s preceding or ensuing EKG. How would you typically manage this rhythm?
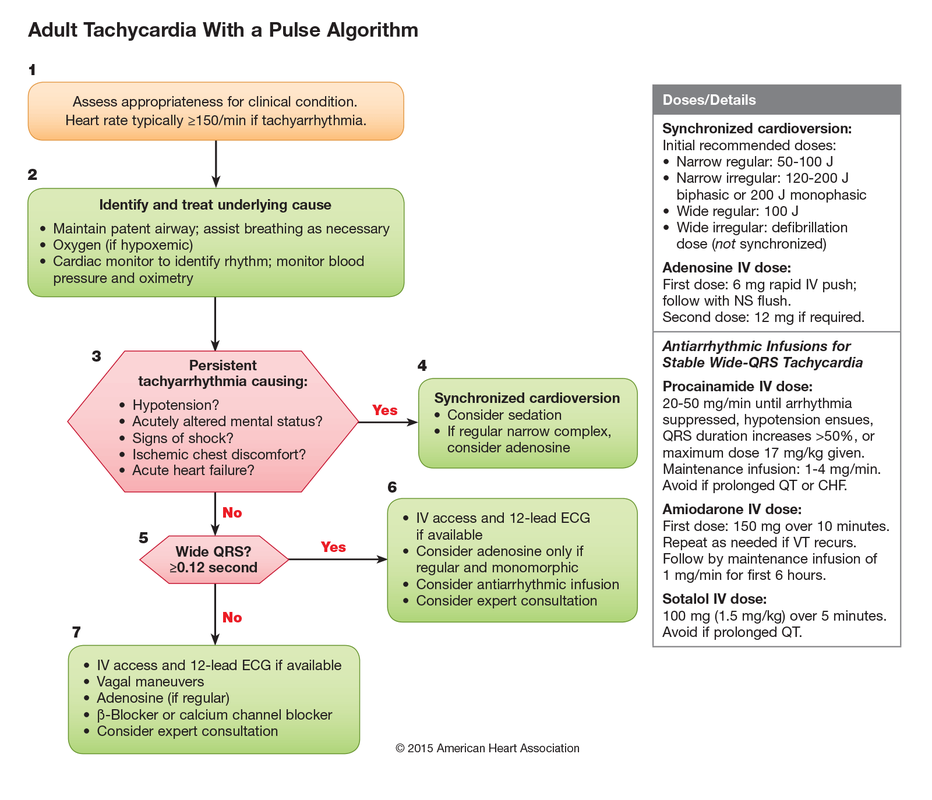
ACLS approach to tachycardias:
1.Does the patient have a pulse? 2. Shockable rhythm or not? If Pulse and unstable → Synchronized cardioversion (the electricity is timed to the cardiac cycle). If the patient is pulseless then analyze the rhythm and determine is it “Shockable” (Pulseless VTach or VFib) or “Non-shockable” (PEA or Asystole). The first step is immediate CPR in both scenarios until you can get the defibrillator to defibrillate the shockable rhythms (electricity not timed to cardiac cycle). ****THESE ARE THE PATIENTS THAT ACLS SAVES**** How would you manage this rhythm in lvad patients?
Call for help when they hit the door. You should NOT perform CPR in an LVAD patient unless you can confirm they are in cardiac arrest. Most often the pump needs troubleshooting. Arrhythmias are not uncommon. You can attempt chemical cardioversion (amiodarone) or electrical cardioversion. Pads do NOT go over the LVAD. Use the anterior/posterior positions.
Take Home Points 1. It is not important to distinguish between types of VFib → the answer is defibrillation 2. Torsades de Pointes can only be diagnosed if the preceding/ensuing EKG has prolonged QT 3. Do NOT perform CPR on LVADs unless Cardiac Arrest confirmed (eg MAP 0 mmHg) 4. When performing defibrillation or cardioversion in LVAD patients place pads Anterior / Posterior Resources: Partyka C and Taylor B. Review article: ventricular assist devices in the emergency department. Emerg Med Australas. 2014 Apr; 26(2): 104-12. Link MS, Berkow LC, Kudenchuk PJ et al. Part 7: Adult Advanced Cardiovascular Life Support: 2015 American Heart Association Guidelines Update for Cardiopulmonary Resuscitation and Emergency Cardiovascular Care. Circulation 2015; 132:S444 61 year old presents to the ED with chest pain radiating to his shoulder What is the diagnosis?
Why Not...
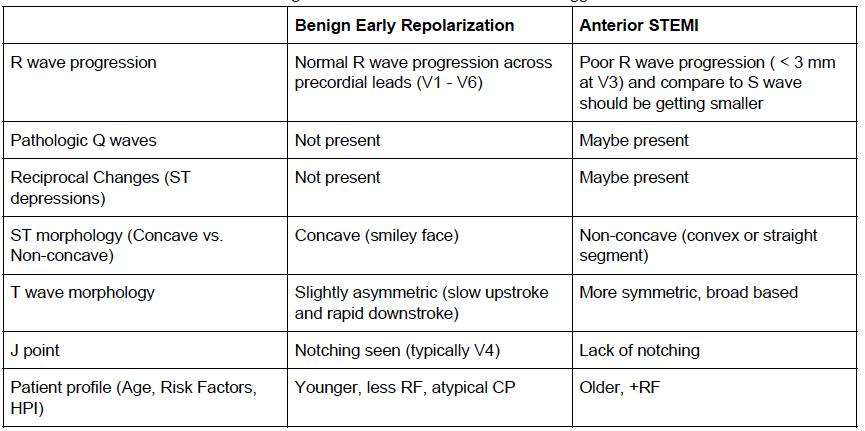
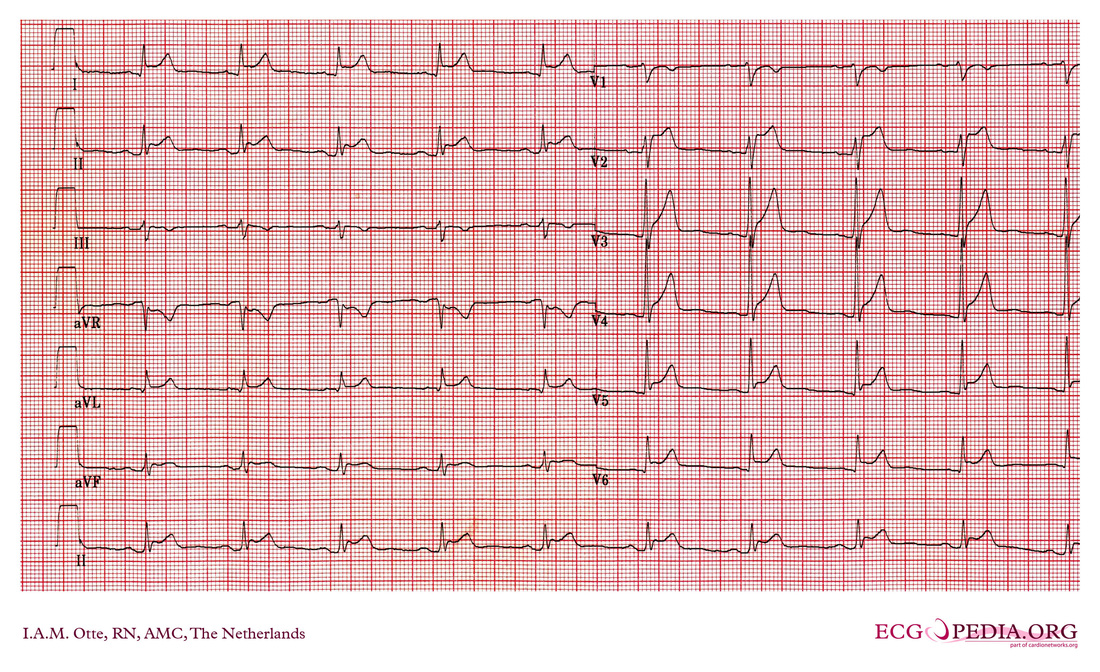
Why is this not Benign Early Repolarization?
The differentiation of benign ST elevations (BER) and Anterior STEMI can be difficult. There are a number of characteristics which are suggestive of BER vs. STEMI. Make sure to examine for other ischemic changes. Our job is to exclude MI and BER should be diagnosis of exclusion. Some features suggestive of each in below table. Learn more
Consider using the Subtle Anterior STEMI calculator in cases where you are concerned, but the EKG may be difficult to decipher Adapted from Katie Januszewicz's Grand Rounds lecture August 30th, 2017 Inflammation of the pancreas can be limited to mild inflammation to severe necrosis of the pancreas and surrounding tissue. Most cases (80%) involve only mild inflammation, however severe pancreatitis can lead to a 30% mortality rate. Most cases are secondary to gallstones or alcohol, but up to 5% of ERCP patients present with post-procedure pancreatitis. Additionally, many medications (120) can cause pancreatitis. In severe cases this can lead to inflammatory responses in nearby tissue and even systemically.
Pancreatitis occurs secondary to an unclear mechanism involving trypsin, a protease that is typically converted from pancreatic trypsinogen in the duodenum. When trypsin is activated in the pancreatic acinar cells, this continues unregulated leading to activation of other digestive enzymes and auto-digestion of the pancreas. Inflammation of the pericardium, usually after a viral infection, presenting classically with chest pain that improves when leaning forward, tachycardia, and dyspnea. Can be associated with a friction rub or pericardial effusion. In pericarditis four stages can be distinguished on the ECG:
Sources:
ECGpedia; http://en.ecgpedia.org/index.php?title=Pericarditis |
Categories
Archive
February 2018
Please read our Terms of Use.
|