|
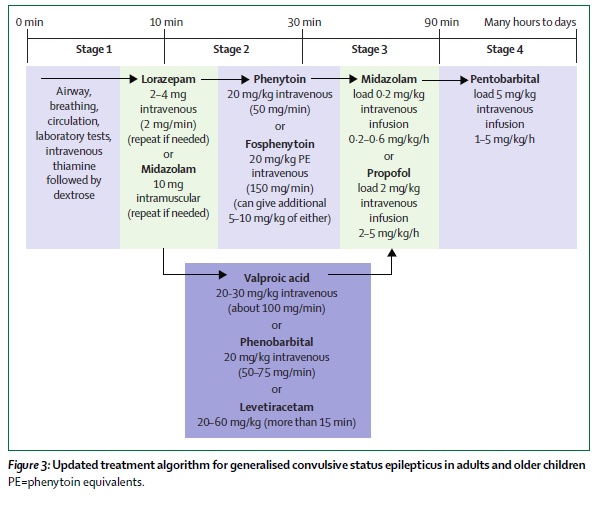
Status epilepticus is a common neurological emergency when a patient has a prolonged seizure or a series of seizures with incomplete return to baseline. The approach to status epilepticus has focused on early seizure termination, and rapid escalation of care to include general anesthesia when needed. Status Epilepticus: A prolonged seizure or multiple seizures with incomplete return to baseline. Treatment of seizures acutely is usually done with IV or IM benzodiazapines. Many studies have discussed the difference between midazolam and lorazepam. The RAPMART study found that intramuscular midazolam is at least as safe and effective as intravenous lorazepam for prehospital seizure cessation. Initial management should also include loading with either phosfenytoin or keppra, in addition to benzodiazapine treatment. If a patient continues to seize despite treatment, consider changing to another benzodiazapine, or escalation in therapy to general sedation. General anesthesia can be undertaken with either midazolam, propofol, or phenobarbitol. There is currently little data to prove if either Keppra or Phospfenytoin are better for preventing additional seizures. Currently, the ESETT trial is underway to determine the most effective and/or the least effective treatment of benzodiazepine-refractory status epilepticus (SE) among patients older than 2 years.
Evaluating Secondary CausesWhen evaluating patients in status epilepticus, ensure a thorough evaluation is done to rule out alternative causes of status. Consider a CT head to evaluate for masses, and consider other 'zebras' such as isoniazid toxicity, infections, tuberculosis, or other causes. Isoniazid toxicity should be suspected in any patient who presents with refractory seizures and metabolic acidosis Proylene GlycolPropylene glycol is a common additive in medications, including ativan, phenytoin, phenobarbital, and other medications. It is metabolized to lactate and pyruvate, and is associated with hypotenision, cardiac toxicity, and renal impairment.
0 Comments
Leave a Reply. |
Categories
Archive
February 2018
Please read our Terms of Use.
|
||||||||||||||||||